Family can make the hard days seem less hard.
Matthew and I took short trip to Washington, DC and while we were gone, Mimi and Papaw, Mumzy and Papa, and Aunt Bam, Uncle Josh, Marshall, Eli, Gabe, and Stella entertained and loved on our 3 kids. All 3 got the love and attention they crave when there are plenty of adults to go around. 1 in particular needed a bit more tending to than the others.
Judah.
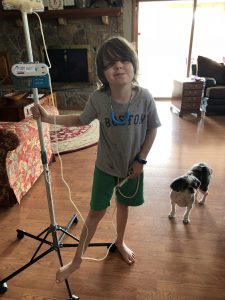
When Matthew and I got back from our trip, we couldn’t wait to hug our kids. We just wanted to give our babies a big hug. When we pulled up to Mumzy and Papa’s house, Emmett and Camilla Kate ran out to greet us. We wrap them up and old them how much we missed them. I looked up from my little girl’s head and saw Judah, sitting not 3 steps from the front door. And it was all I could do to not cry. I gently scooped him up an carried him in the house. Sitting in the wing back, my arms enfolding Judah, I saw a version of him I have never seen. Not in the year leading up to finding our then 4 yr olds brainstem tumor. Not in the 14 months of chemo he suffered through from 5-6 years old. He looked like a ghost of himself. Heavy bags under his eyes, frail, skinny body. Eyes spacey and sad. And he was tired. so tired.
He stayed in my lap for half and hr. Just resting his head on my shoulder, his hand in mine.
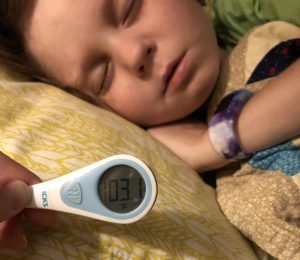
Over then next couple of hrs Matthew and I got the run down on how he had been feeling while we were gone. The jist was, not good. He had begun looking bad on Saturday night, and on Sunday he woke in bad shape. They told us that Sunday he basically moved from the the floor to the couch to floor. He ate nothing. He had no energy or strength. He could not keep anything in his belly even if he wanted to eat. Monday he continued to feel the same way. And it was a holiday. We talked about taking him to the ER. With 2 drs in the house, and an attentive nurse a text away, we had plenty of eyes/ears on his health. The consensus was as long as he is staying hydrated, we could wait until he morning. The night was long. Matthew stayed up with him most of the night, praying over him, watching him breath, helping him to the bathroom.
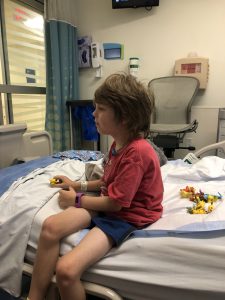
At 9 AM, I called Judah’s Dr she said she wanted to see him. At 12:30 Judah and I got in the van and headed to ETCH Oncology Clinic to see what could be done for him. Thankfully, he was looking a bit better. He had more color in his face. He didn’t have the energy to walk to the clinic so I carried him. However, right before the nurse came back to get us, he decided he wanted to walk to his room himself. He walked as if he was following a zig zag line, not staggering but certainly not straight. But I decided when we first found out about his tumor regrowth that I was going to allow him the independence to do and speak for himself as much as he wanted. So I kept my distance, keeping control of my face so he didn’t see worry.
A couple of hours later, after accessing, blood draws, meds to help stop the diarrhea, and iv fluids, we discovered that, other than typical low labs associated with 48 hours or diarrhea, his labs looked ok. Dr Spiller came in to talk with us. I adore how she begin every visit by talking to Judah. He is her patient after all! She cares so deeply about how he feels, what he has to say, and uses the most friendly and unpatronizing voice each time she address him.
Dr. Spiller: Judah, how are you feeling?
Judah: good
Dr. Spiller: Judah, this isn’t what good feels like. This is what bad feels like.
But honestly that is just how Judah is. 9 times out of 10 the kids will tell you he feels good or is good, even when you KNOW he isn’t. he is compliant and sweet and has a difficult time saying things that may upset ‘his people’. This isn’t super helpful when we, his parents or drs, ask him to tell us how he feels. Or identify what hurts. Or even tell us when he has been sick. He doesn’t see it as lying. He sees it as protecting himself and those he loves from discomfort. I love that about him. It is also scary at times though.
After Dr. Spiller did her exam, we went out in the hall to talk about his weight, nausea, and the need for a feeding tube. She agreed that Judah needed a feeding tube put in asap and wasn’t opposed to a G-Tube instead a NG-Tube. The problems that Dr. Esbenshade described are real. But she said those problems (not healing and getting infected etc) are more common when people are getting chemo every day for long periods of time. When their bodies don’t have time for the blood counts to rebound. But she said that Judah isn’t in that boat. We went over the pros and cons of surgery verses no surgery and in the most lovely way, left the decision up to us. Judah does not want an NG-Tube. He doesn’t want surgery either. But what he wants most, is to just be Judah. And the G-Tube allows him to hide the feeding tube.
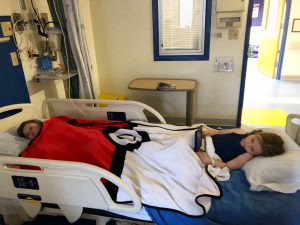
We got home around dinner time, and Judah fell into a great rhythm with his cousins. The fluids did him so much good. Over the next couple of days, Judah did much better, eating and drinking, swimming and playing Wii. He and his siblings and cousins lived it up! And the adults had some much needed connection time. Being seen by your people is one of the great joys of being alive. I long for it and got an overflowing portion.
Judah’s surgery will be Wednesday at noon. He will have to stay for 2 days. And then he will be able to get the nutrition he needs to fatten him up. What a wonderful day that will be!